While historical findings have proved music as a stress reliever and mood enhancer, a recent study reveals that low-intensity sounds impact specific brain circuits and cause pain relief.
Author: Abeer Fatima
The research led by scientists from China and US has outlined the activity of sound-induced brain circuits between thalamus and auditory cortex that play a pivotal role in subsiding pain. These recent findings have opened new doors to discovering more effective methods to manage acute and chronic pain in humans.
Different studies dating back to 60 years proved that music and other low-intensity sounds reduce acute and chronic pain in multiple diseases. To elaborate more, one research in 1960 concluded that music and low-intensity sounds helped alleviate pain in 5000 dental procedures. Since then, scientists have been speculating ways to better understand sound-induced analgesia. Today, music therapy is applied to counter stress, control mood swings, and attenuate post-operative and cancer pain. Despite all these historical findings, a complete neural circuit that reduces pain was yet to be identified, until now.
Uncovering the previous studies, we know that thalamus is a foundational center in the brain that receives pain signals and processes them to other parts of the cortex. Scientists from China hypothesized that thalamus might be the origin of pain signal processing. To further investigate, they induced inflammatory pain in mice and exposed them to three types of soft sounds: a piece of pleasant classical music, unpleasant classical music and white noise. Through several behavioral observations, viral tracing, microendoscopic calcium imaging, and multielectrode recordings, they identified a route from the auditory cortex (AC) to the thalamus that was active when the sound was played at 5 dB, about the level of the whisper. Surprisingly, they found that a lower-intensity sound relieves pain by inhibiting the glutamatergic inputs from the auditory cortex, which limits the pain signals to the thalamus.
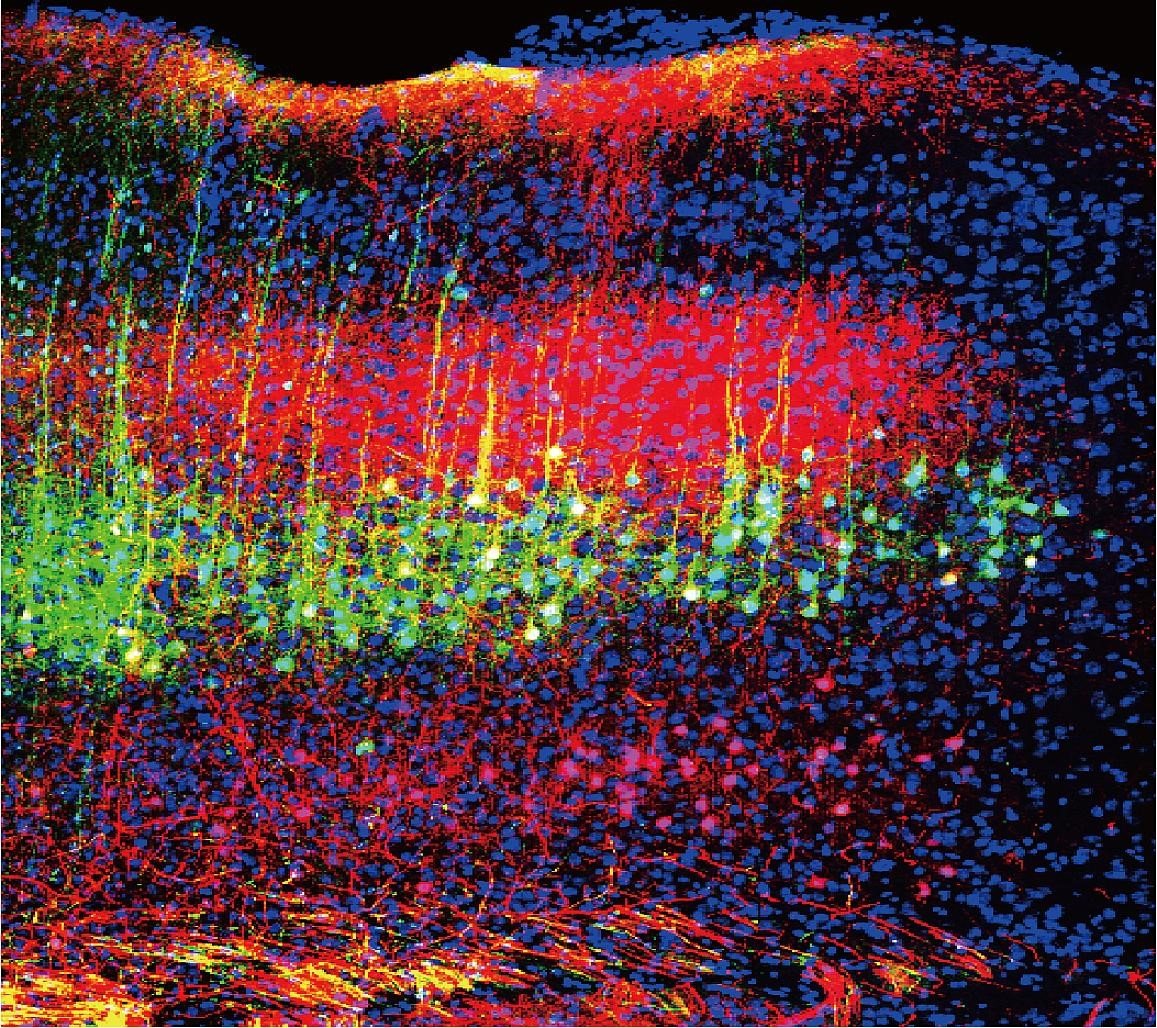
Sound-induced pain relief by lowering the neuronal activity in thalamus (Credits: science.org)
To trace the neural connections, they injected non-infectious viruses with red fluorescent proteins. They observed that with low-intensity sounds, the thalamic region became dense with red fluorescence. The team implanted several multielectrode in mice’s brains. After repeating the experiments multiple times, the imaging revealed that pain signals were specifically diminished between the auditory cortex and thalamic posterior and ventral posterior nuclei. To confirm, they artificially blocked the connections between thalamus and AC using light and small-molecule-based techniques. Consequently, the mice again felt less pain.
According to National Institutes of Health, the NIDCR director Rena D’Souza stated, ‘’By uncovering the circuitry that mediates the pain-reducing effects of sound in mice, this study adds critical knowledge that could ultimately inform new approaches for pain therapy.’’
Modulating pain in humans is not as easy as it seems. Not only does it require technical interventions but also a sound knowledge of pain regulatory mechanisms. Studies like these confer a better understanding of pain-modulating mechanisms and neural processes.
In light of this study, scientists can ultimately explore safer alternative therapies for pain management. However, pain perception in humans is slightly different than in animals, leaving some questions unanswered. Further studies can be designed to monitor thalamic circuits through MRI scans in humans by playing low-intensity sounds. While scientists need to determine whether animal findings apply to humans or not, they also need to investigate the type of sounds that contribute to human pain relief. Some sounds, such as loud bashing or high-pitched sounds, can trigger headaches or even intensify pain, especially migraines. Therefore, researchers need to explore the effects of different sounds on the human brain through advanced technology and conclude safer sounds with controlled intensities that induce analgesia.
References
- Zhou, W., Ye, C., Wang, H., Mao, Y., Zhang, W., Liu, A., Yang, C. L., Li, T., Hayashi, L., Zhao, W., Chen, L., Liu, Y., Tao, W., & Zhang, Z. (2022). Sound induces analgesia through corticothalamic circuits. Science, 377(6602), 198–204. https://doi.org/10.1126/science.abn4663
- Researchers discover how sound reduces pain in mice. (2022, July 7). National Institutes of Health (NIH). https://www.nih.gov/news-events/news-releases/researchers-discover-how-sound-reduces-pain-mice
About the author: Abeer Fatima is a Pharmacy student at Salim Habib University. She is an aspiring content writer whose major interest lies in medicine, science and technology.