The liver is one of the most complex organs of the human body. Its involvement in various metabolic processes and its anatomical proximity to the digestive tract, its blood flow, and its contribution to the detoxification process make it susceptible to a wide variety of disorders.
By Wafa Majeed1, 2, Arooj Kanwal2
Alcoholism, malnutrition, viral infections and xenobiotics cause hepatic diseases which result in a high frequency of patients with liver disease and subsequent increase in the number of deaths from these diseases. Liver steatosis, a condition in which lipid metabolism is disrupted and lipids accumulate in fat droplets within liver cells, is a major complication of obesity, hyperlipidemia, insulin resistance, and alcoholic/nonalcoholic fatty liver disease. If left untreated, benign steatosis can gradually advance to steatohepatitis, fibrosis, cirrhosis, even liver cancer. Therefore, researchers should explore ways to reduce the development of steatosis and study the naturally occurring compounds.
Liver fibrosis is a significant health problem with a worldwide mortality attributable to cirrhosis and primary liver cancer. The last stage of fibrosis, (cirrhosis) occurs mainly in response to viral and toxic-metabolic insults. Chronic hepatitis B, chronic hepatitis C, alcoholic liver disease and nonalcoholic fatty liver disease are the most common causes of fibrosis progression. It is detectable with non-invasive markers which are a few in number but the most investigated and validated biomarkers are the FibroTest (FT), a serum in vitro multivariate assay and a measure of liver stiffness (LSM) using elastography. Anti-viral treatments for hepatitis C and B, reducing alcohol consumption and improving overweight, diabetes and metabolic factors for nonalcoholic fatty liver disease (NAFLD) are the treatments of liver fibrosis, even at the cirrhotic stage. Additionally, prevention of variceal bleeding and detection of small liver cancer in patients with cirrhosis can improve survival.
Cirrhosis development and long term survival are predicted by the presence and severity of fibrosis. According to Epidemiologic studies, the prevalence of NAFLD in the general population have been based on evaluation of fat in the liver using ultrasound, but information on the prevalence of liver fibrosis in the general population is very scarce. Screening strategies for an early diagnosis of liver fibrosis can be designed with this information which may allow therapeutic interventions before the development of cirrhosis.
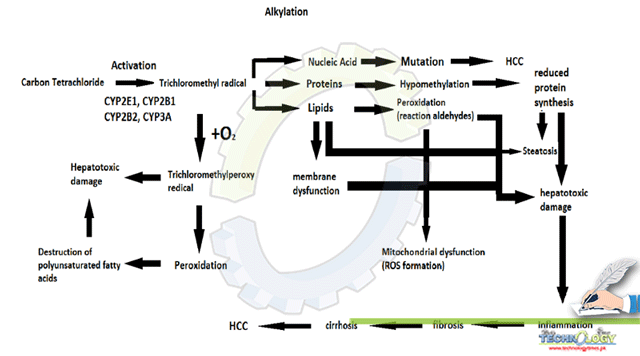
Pathogenic mechanism of liver damage include cytochrome P450 superfamily of monooxygenases (CYP family) metabolizes the CCl4 to the trichloromethyl radical (CClᴣ*) in the liver. Subsequently, this radical reacts with nucleic acids, proteins, and lipids, and impairs key cellular processes which further results in altered lipid metabolism (fatty degeneration and steatosis) and lowered protein quantities (Figure 1). Mutations and the formation of HCC is triggered by DNA and adduct formation between CClᴣ*. Oxygenation of CClᴣ* results in the formation of trichloromethylperoxy radicals (CClᴣOO*) which further initiates lipid peroxidation and the destruction of polyunsaturated fatty acids. Resultantly, the membrane permeability is lowered in all cellular compartments (endoplasmic reticulum, mitochondria and plasma membrane) and generalized hepatic damage characterized by inflammation, fibrosis, cirrhosis and HCC occur.
After hepatic damage, the induction of core signals by fibrogenic reaction in residing and invading liver cells results in the production of reactive oxygen species (ROS), inflammation, apoptosis and hypoxia.
Oxidative stress: Increased production of ROS and a decreased efficiency of antioxidant defendants build a stress that results in chronic liver diseases. This stress stimulates the generation of profibrogenic mediators which are Kupffer cells and other occupant and moving inflammatory cells due to excessive tissue remodeling and fibrogenesis.
Hypoxia: caused by sinusoid capillarisation, vasoconstriction, intrahepatic shunting, thrombosis and compression, is an early fibrogenic stimulus. It blunts mitochondrial functional processes, causes oxidative stress, stimulates endothelial vascular cell growth factor and its receptors, and promotes collagen 1 synthesis in hepatic stellate cells (HSCs).
Inflammation: initiates and controls fibrosis resulting in the release of products for remodeling or degrading the natural basement membrane matrix within the liver.
Apoptosis: Phagocytotic clearance production of apoptotic bodies produces fibrogenic stimuli and triggers pro-inflammatory mediators i.e. Kupffer cells introduce ligands that induce death of normal cells and alpha tumor necrosis factor. Thus, HSCs induce a profibrogenic reaction with the induction of oxidative radicals and up-regulation of Transforming growth factor beta 1 (TGFβ1) factors and collagen 1.
Medicinal herbs and novel therapeutic molecules have emerged as a viable option for the treatment of these hepatic pathologies because epidemiological and clinical studies have shown that the consumption of these compounds is associated with a decrease in the risk of developing liver diseases.
Wafa Majeed1, 2, Arooj Kanwal2
1Department of Pharmacy, University of Agriculture, Faisalabad, Pakistan.
2Institute of Physiology and Pharmacology, University of Agriculture, Faisalabad, Pakistan.