Tuberculosis (TB) is a zoonotic disease having major public health concerns. Zoonotic diseases are those infections that are transferred from animals to humans.
By Prof. Dr. Farzana Rizvi and Hafiz M. Hamza Rasool
According to United Nations Environment Program (UNEP) and International Livestock Research Institute (ILRI), in 2020 about 60% of known infectious diseases in humans and 75% of all emerging infectious diseases are zoonotic. Tuberculosis is an airborne infectious disease caused by a group of closely related Mycobacterium tuberculosis complex (MTBC) species. These species differ in their morphological profiles, host ranges, pathogenicity, geographical distribution, and drug resistance. Mycobacterium tuberculosis complex (MTBC), the primary cause of Tuberculosis in humans and animals, consists of M. tuberculosis, M. bovis, M. africanum, M. microti and M. caprae. Mycobacterium is a facultative intracellular microbe that is non-capsular, non-spore-forming, non-motile, and obligate aerobic thin-rod bacteria. These are usually straight or slightly curved bacteria with a length of 1–10μm and a width of 0.2–0.6μm. Its cell wall is high in lipids, specifically mycolic acid, a thick waxy layer that contributes to bacteria against resistance to numerous disinfectants, antibiotics, and physical damage. In humans, TB is caused by M. bovis via direct or indirect contact (inhalation) and consumption of contaminated animal products or water (ingestion).
Epidemiology of M. bovis in humans
Tuberculosis (TB) is a major global health problem and the leading cause of mortality worldwide with 10 million deaths. It is the second leading infectious killer disease in 2020 after Covid’19, surpassing HIV/AIDS (WHO). In 2020, an estimated 140,000 new cases of zoonotic tuberculosis were recorded worldwide, with 12,500 fatalities owing to the disease with Asia and Africa having the greatest frequency. M. bovis is thought to be responsible for 10-15% of new cases of human tuberculosis in developing countries. Bovine tuberculosis (BTB) is common in Africa and Asia (Pakistan, India & Afghanistan) and its real incidence in the human population of these countries is poorly known.
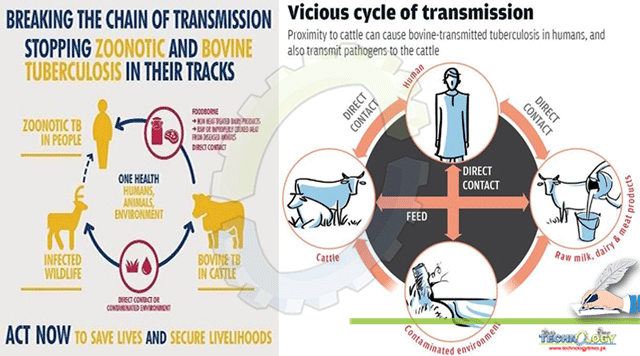
Transmission of M. bovis in humans
Humans acquire M. bovis infection from cattle directly by erogenous route or through direct contact with materials contaminated with the secretions of an infected animal. People in specific occupations such as veterinarians, farmers, zookeepers, milkers, animal dealers, and abattoir workers are at high risk. People in these occupations may develop pulmonary tuberculosis from M. bovis and in turn, put other human and susceptible animals at risk. Indirectly, man acquires the diseases from animals by consuming unpasteurized infected milk and ingestion of meat and meat products of slaughtered infected cattle.
Clinical Manifestation of Tuberculosis
- bovis infection in humans has similar clinical forms as those caused by M. tuberculosis. Most cases have a gradual, non-alerting start that varies depending on the virulence of the causing infection, the patient’s age, the organ affected, and the host immunological condition. It has been suggested that the common clinical manifestation of M. bovis infection in humans is majorly associated with the extrapulmonary form of the disease like Pleural TB, Lymph nodes TB, Genitourinary TB, and Bone TB. Systemic symptoms include fever, lack of appetite, weight loss, asthenia, copious nocturnal sweating, and overall malaise. Organ-specific symptoms vary by organ and illness location: Tuberculosis of the lungs (dry or productive cough, hemoptysis, pleuritic pain, dyspnea and pneumonia), Pleural TB (Pleuritic chest discomfort, low-grade fever, dry cough, worsening of health, weight loss, and increasing dyspnea), Lymph nodes TB (painless swelling develops in the cervical and supraclavicular area), Genitourinary TB ( pollakiuria, dysuria, hematuria and flank pain) and Bone TB (inflammation of the peripheral joints, tuberculous meningitis with anorexia, malaise, headache, consciousness, neck stiffness, and nausea).
Diagnosis
Bovine tuberculosis in live animals is usually diagnosed based on delayed hypersensitivity reactions. Diagnosis of active TB in people is based on interferon-gamma release assay (IGRA), immunoglobulin G-test, sputum smear examination, and some rapid gene assays like Xpert MTB/RIF. But these commonly used tests are not able to differentiate M. tuberculosis complex into the distinct species of M. tuberculosis and M. bovis. Therefore, most cases of zoonotic Tb are misclassified. The identification of M. bovis in humans can be done by PCR and gene sequencing of culture isolates, but for these tests, the proper collection of samples is very essential.
Treatment
The treatment and recovery of patients with zoonotic tuberculosis are difficult. Patients with zoonotic TB may get suboptimal therapy because most healthcare professionals begin treatment without doing medication susceptibility testing. As a result, zoonotic tuberculosis is underdiagnosed. BCG vaccination is the only TB vaccine approved for use in humans against pulmonary tuberculosis in children and adults with a cure rate of 0–80%. Because M. bovis is completely resistant to pyrazinamide, a major first-line TB treatment therefore precise illness diagnosis and distinction are critical. Isoniazid, streptomycin, para-aminosalicylic acid combos are routinely used to treat human TB. The need for long-term medication for the condition can lead to the emergence of multidrug-resistant (MDR), exceptionally drug-resistant (XDR), and even fully drug-resistant (TDR) bacterial strains. Most MDR-TB medication regimens now contain an aminoglycoside (e.g., streptomycin, kanamycin, amikacin) as well as a fluoroquinolone. DOTS (directly observed treatment short course) is a very efficient and cost-effective TB control approach that is widely approved by WHO.
Control
Zoonotic TB has a significant economic impact on international commerce, animal productivity (e.g., lower meat output, low reproductive rate, and low milk yield), human health costs, and compensation from control programs. The disease load in people cannot be minimized until food safety standards are improved and bovine tuberculosis is controlled in animals. To eradicate bovine TB, identify critical demographics and TB transmission risk routes, slaughterhouse monitoring, mandatory milk pasteurization, “test and slaughter” laws, effective education and suitable hygiene practices should be appropriately implemented. The National TB control program of Pakistan (NTP) aims to achieve a TB-free Pakistan by 2025, lowering the prevalence of tuberculosis in the general population by 50% compared to 2012, by providing universal access to high-quality TB care and eliminating TB deaths. Therefore, it is the need of the hour to add zoonotic tuberculosis in the National Tuberculosis control program to control and eradicate bovine tuberculosis and make Pakistan a Tuberculosis free country.