Antimicrobial development is considered as one of the major advances in the field of medical science. Antimicrobials are the medicines which are used to treat infections caused by microorganisms in humans, animals and plants, and have saved millions of lives.
By Arfa Tehreem, Arooj Fatima, Ayesha Shareef, Fouzia Parveen
Since the day of the development of antimicrobials, they are excessively used for the treatment of many microbial diseases that would otherwise be impossible. But the excessive use of antimicrobials may lead to the development and dissemination of antimicrobial resistance. Antimicrobial resistance is a major threat to public health in the whole World. And now we are living in the post antibiotic era where it is very difficult to treat many infections due to rapidly increasing antimicrobial resistance.
Why antimicrobials are used for food animals?
World’s population is tremendously increasing day by day and the demand for more food increases. Before the development of antimicrobials most of the food animals died due to many microbial diseases but the use of antimicrobials prevents many diseases and plays a vital role in protecting the health. Antimicrobials also play a major role in livestock production. They are used for the prevention and treatment of disease as well as for the growth promotion of food animals. For many years we have enjoyed the benefits of antimicrobials but the irrational and irresponsible use of Antimicrobials cause antimicrobial resistance.
Antimicrobial residues and factors which develop resistance in food animals:
Residual amount of antimicrobials found in the edible portion of animal products after slaughtering the animals are called antimicrobial residues. If antimicrobials are not used properly, they may accumulate in food as residues. And when these foods are consumed by humans, they transmit to them and can result in severe consequences in humans.
Over prescription of antimicrobials, poor sanitation and hygiene for both humans and animals, poor infection control in health care settings, poor access to quality, affordable medicines, vaccines and diagnostics, lack of awareness and knowledge and lack of enforcement of Legislation cross-contamination with antimicrobial resistant bacteria during food processing are the factors which contribute to the development of antimicrobial resistance in food animals.
Transmission of resistance to human through food animals:
- Food producing animals develop resistant bacteria in their gut when antimicrobial substances are used for therapy in them or for prophylaxis of infections or as a growth factors administered in their feed. Drug resistant bacteria remain on the food products of these animals that can be eaten by humans.
- Raw food products can be consumed without processing or preservation and therefore hold a substantial risk for the transfer of antimicrobial resistance to humans, as the eventually present resistant bacteria are not killed. Also the transfer of antimicrobial resistance genes between bacteria after ingestion by humans may occur and spread the risk of resistance.
- Under minimal processing or preservation treatment conditions, sub lethally damaged or stressed cells can be maintained in the food, inducing antimicrobial resistance build-up and enhancing the risk of resistance transfer. Food processes that kill bacteria in food products, decrease the risk of transmission of antimicrobial resistance.
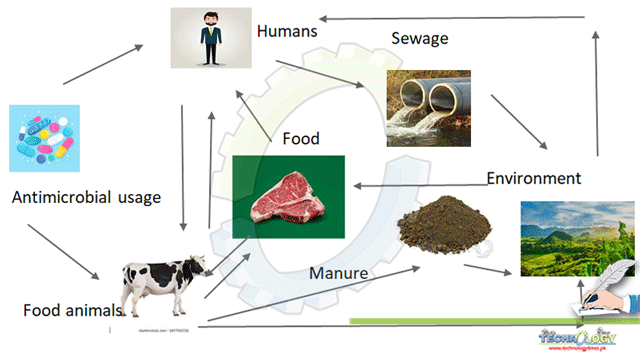
Pathways for the transmission of antimicrobial resistance from food animals to humans and their environment
Detrimental effects of antimicrobial resistance:
Once antimicrobial resistance develops in humans, they impose very serious health issues. People with an antibiotic resistant infection get sick for longer time and are more difficult to treat. Most of the people die from antibiotic resistant infections as they cannot be treated with available antibiotics. The worst case is that we no longer have effective antibiotic to treat such infections. To treat antimicrobial resistant infections, we require other antibiotics which have harmful side effects. People with antimicrobial resistance infections may require more complex care and longer hospital stays. They need more expensive health care and medications and have higher risk of transferring the disease to other immune compromised individuals. But the good news is that antimicrobial resistance is reversible. We can reduce the risk of antimicrobial resistance by only using antibiotics appropriately and as prescribed.
Antimicrobial resistant zoonotic pathogens present on food constitute a direct risk to public health. The indiscriminate use of antimicrobial lead to drug resistance which threaten the health of both animals and humans. Antimicrobial resistance in food animals has impact on animal health as well as associated with resistance infection in human. Resistant bacteria in animal may directly or indirectly reach human through food. Homologous relationship between drug resistant bacteria in human and animal have been identified in most common food borne pathogen such as E.coli and Salmonella and Methicillin resistant Staphylococcus aureus.
Methicillin Resistant Staph Aureus has been found in mutton, pork, chicken, and other meat products. Salmonella enteritis and its analysis confirm that chicken sandwiches were the source of infection.
Following are the examples of resistant bacteria which are transmitted to humans through the consumption of food animals:
|
Resistant bacteria pathogen |
Type of animal derived food |
Nature of antimicrobial resistance |
|
E.coli |
Meat |
Tetracycline |
|
Methicillin resistant Staphylococcus aureus (MRSA).
|
raw milk from cattle, sheep and goat |
Multi drug resistance(MDR) |
|
Salmonella |
Chinese pork |
Multi drug resistance(MDR) |
How we can reduce the risk of antimicrobial resistance through food animals?
It is very crucial to educate people about the danger of antimicrobial resistance and how we can reduce the risk of it. In humans resistance to different antibiotics develop through the consumption of food which have previously been treated with antibiotics. As the antimicrobials are not used appropriately and as prescribed the residues of them may be present in them and when those foods are consumed by humans, they cause resistance to the same antimicrobial in humans.
Antimicrobial resistance food borne illness also spread the same way as other food borne illnesses. We can take different preventive strategies to control antimicrobial resistance to protect ourselves and our family. A simple way is that we can adopt following preventive measures to reduce the transmission of resistance from food to humans.
Follow simple food safety tips:
1- Washing hands at workplace i.e. cutting board, dishes and utensils before and after handling with any raw food.
2- Washing hands after touching raw meat, poultry, seafood or their juices and uncooked eggs.
3- There are many resistant microbes on uncooked raw meat which when come in contact with other ready to eat foods, fruits and vegetables may contaminate them. So separate raw meat from fruits and vegetables.
4- Make sure that the meet is properly cooked at safe internal temperature which is 145°Ffor beef,160°Ffor ground red meat and 165°F for poultry.
5- Washing hands after touching animals and pets or their belongings (bowls and toys) or food, water and habitat of animals.
6- Purchase meet and other animal derived food from those producers who use proper hygienic measures with minimal antimicrobials.
7- Use antimicrobials for food animals only when needed and prescribed by doctor or veterinarians.
8- Dispose of the expired antimicrobial properly, as the antimicrobials present in trash may be eaten by animals and may accumulate as residues in them and through food chain may transmit to other animals and humans.
9- To store cooked food, keep it in the refrigerator between the temperature of 0C and 5C. If food is not stored at this temperature the bacteria will be able to multiply and contaminate the food.
10- Reheat cooked food properly at 75C to kill any resistant bacteria which manage to grow during the refrigeration period.
11- Vaccinate animals to reduce the need for antibiotics and develop alternatives to use of antibiotics in animals.
Transmission of antimicrobial resistance through food animals is an alarming issue. So, we should avoid those circumstances that results in antimicrobial resistance. People should adopt the necessary precautions to minimize the impacts of antimicrobial resistance on human health. Countries should follow the World Health Organization, World Organization for Animal Health, and the Food and Agriculture Organization of the United Nations recommendations to implement national action plans encompassing human, food animal, and environmental sectors to improve policies, interventions and activities that address the prevention and containment of antimicrobial resistance from farm-to-fork.
Authors: Arfa Tehreem, Arooj Fatima, Ayesha Shareef, Fouzia Parveen, University of Veterinary and Animals Sciences, Lahore