Elementary mercury makes up to one half of dental amalgam by weight, with the rest made up of other metals such as silver and copper.
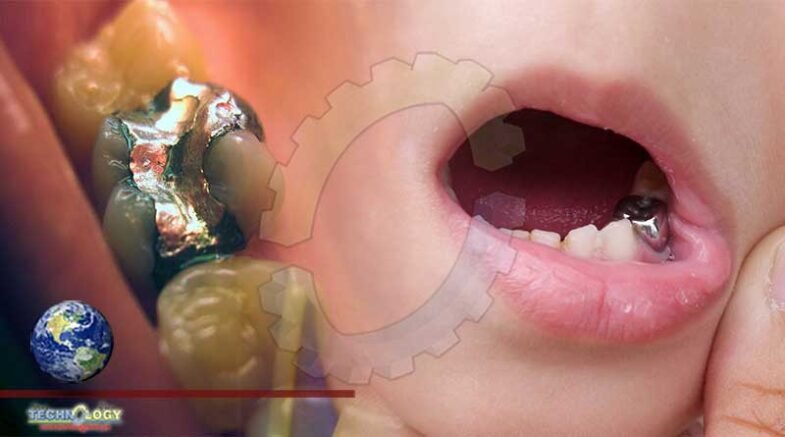
We’ve all heard that mercury is poisonous — causes neurological damages, developmental defects, etc. Mercury thermometers have been phased out and replaced with non-mercury ones. But not so with dental amalgam (silver filling for cavities), which contains mercury, even though comparable alternatives are available. Some of us continue to have amalgam in our mouths, and some dentists continue to put it in our mouths.
Mercury exists in three forms — elemental mercury, inorganic mercury, and organic mercury. Elemental mercury is the form used in thermometers and dental amalgams. Elementary mercury makes up approximately one half of dental amalgam by weight, with the rest made up of other metals such as silver, tin, and copper. Elemental mercury is a shiny liquid and evaporates at room temperature. Elemental mercury is toxic primarily through inhalation. Long-term complications of elemental mercury exposure include neuropsychiatric effects (tremor, anxiety, emotional instability, forgetfulness, insomnia, fatigue, disturbances of thought and movement) and kidney damage. Whether chronic exposure to elemental mercury (such as through dental amalgam) increases the risk of reproductive or developmental damage is unknown.
Because it releases low levels of mercury vapor over time in the mouth, dental amalgam has sparked health concerns and lawsuits against dentists and amalgam manufacturers. However, it has been the position of public health organizations and dental organizations worldwide that dental amalgam is safe.
Science continues to evolve. The FDA recently updated recommendations regarding dental amalgam. While maintaining that dental amalgam is safe for general population, the FDA now “strongly encourages” that certain high-risk groups avoid getting dental amalgam, and use non-mercury alternatives (such as composite resins and glass ionomer cement fillings) whenever possible. These high-risk groups include:
· Pregnant women and their developing fetuses;
· Women who are planning to become pregnant;
· Nursing women and their newborns and infants;
· Children, especially those younger than six years of age;
· People with pre-existing neurological disease such as multiple sclerosis, Alzheimer’s disease or Parkinson’s disease;
· People with impaired kidney function; and
· People with known heightened sensitivity (allergy) to mercury or other components of dental amalgam.
The FDA pointed to “uncertainties in the most vulnerable patients,” noting that: 1) developing neurological systems in fetuses and young children may be more sensitive to the neurotoxic effects of mercury vapor; and 2) the amount of vapor released can also depend on the age of the filling as well as a person’s habits such as teeth grinding.
Importantly, the FDA recommends against anyone removing or replacing existing amalgam fillings in good condition unless it is medically necessary, because removing intact amalgam fillings can cause a temporary increase in exposure to mercury vapor and a potential loss of healthy tooth structure, “resulting in more risks than benefits.”
In response, the American Dental Association issued a statement that it reaffirms its position that dental amalgam is “durable, safe, and effective.” The ADA stressed there “was no new scientific evidence cited as part of the FDA recommendation.”
Of note, in its updated recommendation, the FDA did refer to evidence gathered during the November 2019 meeting of the Immunology Devices Panel of the Medical Devices Advisory Committee. The white paper from this event notes that “there is not sufficient evidence of a relationship between clinically detectable adverse health outcomes and dental amalgam mercury exposure.” The FDA noted uncertainties regarding the available evidence due to the lack of information on the origin of the various species of mercury, and called for further examination.
Toxicity is a matter of amount. Anything is poison when it exceeds a certain level. On the other hand, we are exposed to various toxins at levels too low to have toxic effects. But what effect would a low-level, long-term exposure have on a vulnerable subpopulation? Science cannot always provide a black-and-white answer. Sometimes it’s because there is no data or only limited data — or because the risk depends on many different factors. In such a case, we stand by science, do our cost-benefit analysis, and make a judgment call.
Originally published at JD Supra
