Can you imagine a life without your favorite dairy products? Coming home on a hot summer day and not being able to enjoy ice-cream or a glass of shake sounds pretty bad.
 What is even grimmer is having to eat pizza without cheese!! These are just some diet restrictions that people with lactose intolerance have to observe. Lactose intolerance is a condition in which the individual experiences gastrointestinal symptoms such as abdominal pain, bloating, diarrhea, excessive flatulence and in severe cases, cramps and nausea.
What is even grimmer is having to eat pizza without cheese!! These are just some diet restrictions that people with lactose intolerance have to observe. Lactose intolerance is a condition in which the individual experiences gastrointestinal symptoms such as abdominal pain, bloating, diarrhea, excessive flatulence and in severe cases, cramps and nausea.
Lactose maldigestion or hypolactasia can appear either as a result of genetic makeup or due to an infection resulting in severe damage to intestinal mucosa. Since lactose is a common disaccharide and a part of many foods of daily consumption, it is of utmost importance that a person showing sensitivity to lactose be well aware of his specific body needs.
Some lactose intolerant individuals can consume milk and dairy products without developing the symptoms, others however need some kind of lactose restriction. The nature of symptoms and severity is purely personal and changes with age and various physiological conditions.
Despite of the fact that lactose is the most important source of energy for an infant, providing more than half of the total energy requirement, yet it has no special nutritional importance for adults.
This disaccharide is extensively used in food industry for instance in various sweets, confectionery, bread and sausages because of its property to bind with water and give the specific food a good texture and color. Fun fact that as far as sweetness is concerned, lactose is one third as sweet as saccharose and less than half as sweet as glucose.
How does lactose sensitivity work?
Lactase enzyme present in the microvili of small intestine is responsible for splitting and hydrolyzing the lactose taken through diet into glucose and galactose. These monosaccharides are then assimilated into the body. Improper absorption of lactose can take place due to two reasons: either complete absence of lactase termed as Alactasia or deficiency of lactase termed as Hypolactasia.
This can result in increased influx of fluids into the bowel resulting in diarrhea like conditions, as shown in the figure 1. Furthermore, the lactose is acted upon by bacteria present in the colon. This fermentation results in cleavage of lactose into monosaccharides which also draws more fluids into the bowel along with the release of gaseous by-products.
Figure 1
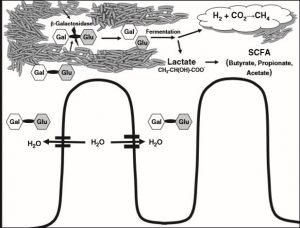
The presence of disaccharides in the jejunum causes influx of water and fluids leading to diarrhoea like conditions. Fermentation of lactose results in production of fatty acids and gases like carbon dioxide (CO2), hydrogen (H2) and methane (CH4).
What are the different types of lactose sensitivities?
There are generally three basic types of hypolactasia; primary, secondary and the extremely rare congenital Alactasia. Primary adult hypolactasia is the most prevalent. It is characterized by presence of relatively low levels of Lactase and develops during childhood at various ages. Secondary Lactase deficiency results from infection or injury to bowel mucosa.
There can be many reasons for that, such as acute gastroenteritis, persistent diarrhea, small bowel overgrowth, cancer chemotherapy etc. congenital alactasia is a rare autosomal recessive enzyme defect in which the infant has no expression of Lactase from birth and therefore cannot digest breast milk.
With the development of soybean derived infant formulas and lactose free dairy products in the 20th century, the survival rate of infants born with congenital alactasia increased. There is also a newly defined type of hypolactasia known as developmental Lactase deficiency. In this type, the symptoms are observed in preterm infants of less than 34 weeks of gestation.
What are the trends?
A normal individual loses 90 to 95 percent of birth Lactase levels by early childhood and the levels continue to decline throughout life. As a result of surveys conducted to find the prevalence of hypolactasia in different ethnic groups, a range of results were obtained. It was found that only 2% North Europeans have this condition while nearly 100% adult Asians and American Indians are prone to be lactose intolerant.
The ethnic groups with African roots had a prevalence of 60 to 80% while Latinos showed 50 to 80% positive results. Due to the presence of such a huge number of people experiencing poor digestion of lactose and lactose containing foods, it is often argued that lactose sensitivity is a “natural” or “normal” phenomenon that occurs with age.
How can it be diagnosed?
There are two main methods by which lactose intolerant individuals can be screened; direct and indirect. The direct methods include measuring the levels of mucosal disaccharides in the intestines. Indirect methods include various breath tests like the breath hydrogen test, the measurement of breath 13-CO2 after consumption of 13C-lactose and checking breath radioactivity after 14C-Lactose ingestion.
Hydrogen, methane and carbon dioxide is produced when intestinal bacteria consume lactose and break it down to fatty acids and gaseous by-products (Figure 1). Urine tests which measure levels of galactose using an enzyme strip are also employed for the diagnosis of hypolactasia.
Measuring stool pH and paper chromatographic tests for recording sugar levels in the faeces are less reliable tests and are not recommended. Lastly, a good clinical history may prove to be very important in linking the symptoms with presence of this condition.
How can it be managed?
Being lactose intolerant doesn’t mean that the individual is allergic to milk. Milk sensitivity in fact arises when the body reacts towards the proteins present in the milk. The degree of lactose sensitivity differs in each individual and is very personal.
That is why the diet restrictions that should be observed in order to avoid symptoms should be based on the individual’s experience and clinical history. Most patients do not require a totally lactose free diet and it is in their best interest too. Why? Because dairy products are the key source of calcium (75%), vitamin A and D, riboflavin and phosphorus in our diet.
It is recommended to the adult patients to keep a regular intake of calcium supplements ranging from 1200 to 1500 mg per day. Milk consumption is commonly limited to about 250 to 373 mL per day.
Using lactose reduced milk, soy milk or rice milk and avoiding medications that use lactose as a filler are also helpful ways in which we can avoid the development of symptoms. Individuals with hypolactasia should be educated regarding their sensitivity.
Workplaces and restaurants or common food places should be made user friendly for patients following a strictly restricted diet. Gastrointestinal symptoms due to milk are very common and quite often may occur regardless of any sensitivity to lactose. It is very important to carefully diagnose hypolactasia before any diet restrictive steps are taken.
Several authors consider the condition to be overrated or hyped up due to the varying amounts of the degree of symptoms that occur in patients. This range of symptoms however does not imply that people experiencing poor lactose digestion should be overlooked, because for them the symptoms are painful and exhausting. Research has been done and is still being continued in this field to find better diagnostic methods that we can use in our routine life.
Although hypolactasia rarely leads to life threatening symptoms, it is still responsible for a great deal of discomfort for the patients. Disrupted quality life, loss of attendance, leisure, sports activities and work time can be a major cause of annoyance for patients.
Therefore it is important to address the symptoms from an early age. We should provide not only the appropriate education to the masses regarding the condition but also encourage them to be supportive and cooperative towards such individuals.
Authors: Hafsa Ahmed Khan and Muhammad Mustafa