Polycystic ovary syndrome (PCOS) is considered one of the most common hormonal disorders of women in reproductive age. PCOS was first described firstly by Stein and Leventhal in 1935.

According to the National Institute of Health (NIH 1990), it is characterized by chronic anovulation and clinical or biochemical evidence of hyperandrogenism. PCOS is a group of symptoms that affects the ovaries and ovulation.
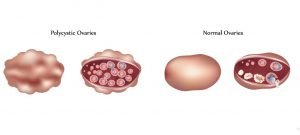
In PCOS, many small, fluid-filled sacs grow inside the ovaries. These sacs are actually follicles, containing an immature egg. The eggs never mature enough to trigger ovulation. The lack of ovulation alters levels of estrogen, progesterone, FSH, and LH. Estrogen and progesterone levels are lower than usual, while androgen levels are higher than usual.
- Causes of PCOS
Insulin resistance, hormonal imbalance and genetics may be considered as a factor of causing PCOS. Although the exact cause of PCOs is not known but still it is thought to be related to hormonal imbalance. Thus, Irregular menstrual cycles, insulin resistance, hyperandrogenism, changes in mood, depression are some characteristics of PCOS.
- Insulin Resistance
Insulin is a hormone which is released by pancreas to control blood glucose levels by making the glucose to move inside the cells so it can be used as a fuel for energy production. Insulin resistance is a core pathophysiology of polycystic ovarian syndrome in which body cells can’t use insulin properly and the body’s demand for insulin increases.
Thus, more insulin is produced to compensate and this extra insulin triggers the ovaries to produce excess amounts of male hormones like androgens (testosterone); which ultimately affect the follicular development and hence interrupts with normal ovulation.
- Hormonal Imbalance
The hormones which become imbalance during this disease include testosterone, LH, prolactin and SHBG (sex hormone binding globulin). The exact reason of their imbalance is not known.
But still it is considered that it might be due to problems related to ovary itself or the other glands which are responsible for production of these hormones and it might be due to parts of brain which control their production. One another reason of hormonal imbalance is insulin resistance which disrupts the hormonal balance.
- Genetics
The risk of having PCOS become increased if it is already present in families like if your mother, your sister and your aunt are suffering from PCOS already then you will be at greater risk of having PCOS. This suggests that there may be a genetic linkage although no specific genes have yet been identified.
- Symptoms of PCOS
The symptoms of PCOS may begin to occur shortly after puberty or in late teens or it may also occur during early adulthood. But sometimes symptoms of PCOS may go unnoticed as these symptoms are attributed to other causes also.
The crucial symptoms by which PCOS can be diagnosed may include; weight gain, hirsutism (unwanted hair growth on facial regions, lower abdomen, and back and on chest region), acne, infertility, pelvic pain, mood swings and sleep apnea.
According to UK charity, one of the five women suffers from polycystic ovary syndrome (Verity, 2017). There is currently no cure for PCOS but there are some strategies which can help to manage the symptoms of PCOS. It is thought that one of the simplest and most cost-effective treatments for PCOS is to boost the intake of vitamin D and calcium.
- Role of vitamin D and calcium
Vitamin D is a steroid hormone that is primarily known for its role in skeletal health and calcium homeostasis. Vitamin D is vital for many bodily functions like; it has anti-cancer effects, improves immune system functioning to help to fight against infection, improves muscle functioning and improves blood circulation.
Vitamin D helps the body in absorption and metabolism of calcium and phosphorus to build strong bones and teeth. Besides vitamin D; calcium helps in muscle contraction, maintenance of cell membranes, clotting of blood and normal functioning of nerves, muscles and heart.
The absorption of calcium in human body is associated with vitamin D. So, with respect to many vital functions of the body, both vitamin D and calcium have equal importance.
- Consequences of vitamin D deficiency
The prevalence of vitamin D deficiency in women with PCOS is about 67-85 per cent, with serum concentrations of 25(OH) D <20 ng/ml. It is newly accepted concept that the metabolic changes in PCOS are related to dysfunction of vitamin D and calcium metabolism, which is important in follicular development and normal glucose metabolism.
Most of the cells in our body have vitamin D receptors on them which depict that vitamin D is not just a vitamin but also a hormone. Its deficiency not only causes poor bone mineralization but it also contributed in severe complications.
Vitamin D deficiency has been related to a number of non-skeletal disorders which includes; obesity, insulin dysregulation, dyslipidemia, hypertension, cardiovascular diseases, autoimmune diseases, and cancers.
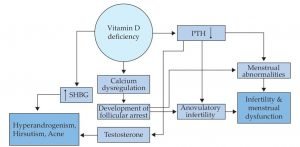
Fig: 1 Consequences associated with Vitamin D deficiency leading to symptoms of PCOS:
- Complications of PCOS with vitamin D deficiency
Vitamin D deficiency is highly prevalent in sufferers of PCOS and it is linked to the metabolic complications which are associated with the disease. There is increasing evidence that vitamin D affects insulin and glucose metabolism, and a low vitamin D status is suspected to be a risk factor for impaired glucose tolerance, insulin resistance and T2DM.
Multiple studies have shown that PCOS patients, particularly if obese, have lower serum vitamin D levels and have been associated with hyperandrogenism, metabolic syndrome, insulin resistance, and increased body mass index (BMI).
A low vitamin D concentration results in an elevated serum level of parathyroid hormone (PTH), and increased PTH concentrations are suspected to be involved in glucose metabolism and decreased insulin sensitivity6. The effectiveness of calcium and vitamin D is mainly due to their effect on body weight and follicular maturation.
Both calcium and Vitamin D deficiency are considered as potential risk factors for obesity. In addition, it is well considered that increased body weight has a considerable negative effect on Vitamin D concentrations in women with PCOS. The role of Vitamin D in the reproductive system has been demonstrated in several studies.
Impaired calcium regulatory system could cause follicular arrest. Moreover, animal studies in this field indicated that the calcium has a crucial role in oocyte maturation as well as resumption and progression of follicular development.
One research revealed that 1,25-dihydroxyvitamin D mediates an enzyme known as aromatase which converts androgen derivatives to estrogen in granulosa cells of the ovaries.
Therefore, dysfunction in this mechanism affects the menstrual cycle and ovulation by altering the hormone levels mediated. To validate some of these outcomes, researchers have also experimented in treating PCOS patients with vitamin D and calcium supplementation.
Role of Vitamin D in improving complications of PCOS
- Improves Fertility
According to one study which was published in the Journal of Obstetrics & Gynecology; the infertile PCOS women who were supplemented with 1000 milligrams of calcium and 400 international units (IU) per day of vitamin D had shown improvements in menstrual regularity after 3 months of supplementation of vitamin D and calcium.
Thus, vitamin D is considered to play a vital role in development of egg, ovulation and overall fertility. Vitamin D receptors are found in the placenta, ovary and uterine lining suggesting that Vitamin D plays an important role in complications regarding female reproductive system. The research shows that women with Vitamin D deficiency have do not respond as well to ovarian stimulation with Clomid (an oral medication to stimulate ovulation).
As blood concentrations of Vitamin D rises, the pregnancy success rates then also rise. If you are trying to conceive with PCOS, it may be worthwhile adding Vitamin D to your supplement course. Vitamin D status has also been shown to improve fertility and success rates of pregnancy during assisted reproduction therapies.
According to European Journal of Endocrinology, the infertile women who were provided with Clomid stimulation along with vitamin D supplementation, had shown much more mature follicles and were more likely to conceive as compared to infertile women who were only given with Clomid stimulation had less mature follicles and lower pregnancy rates .
- Improves Metabolic Markers
There is an inverse relationship between vitamin D and metabolic risk factors such as insulin resistance, level of testosterone, cholesterol, triglycerides and weight. It means that when vitamin D status raises the metabolic factors including insulin resistance, testosterone level and weight decreases.
A study published in Journal of Clinical Nutrition, showed that overweight women with PCOS who were vitamin D deficient and took vitamin D supplementation for eight weeks had significantly shown improvements in insulin, triglycerides and cholesterol levels.
Furtherly, one study of Pal and colleagues have shown that supplementing with vitamin D and calcium for 3 months significantly reduced testosterone levels in women with PCOS.
- Improves Depressive Mood
Living with PCOS is not easy. The sufferers of PCOS often have low self-esteem, feel ugly, suffer from emotional stress, poor perception of their body image and become depressed by struggles to conceive. Moran and colleagues found that vitamin D deficiency was a significant independent predictor of depression in both women with or without PCOS.
Vitamin D deficiency has been linked with higher incidences of mood disorders like premenstrual syndrome, seasonal affective disorder and depression. Although no research has been done specifically on how vitamin D supplementation helps the mood of women with PCOS in particular.
But as we can see the adequate amounts of vitamin D has a significant role in improving the complication liked with PCOs. So, when we get relief from the burden of PCOS we certainly get rid of depressive mood, frustration and anxiety.
So, just to sum it up vitamin D supplementation is important for women with PCOS because it helps improves fertility, possibly improves mood, might help symptoms of hyperandrogenism and improves insulin resistance.
- Daily requirement of vitamin D
The Vitamin D council recommends that you need about 5000 IU per day. As the normal average level of vitamin D in the blood is 50-100 ng/ml.
Conclusion
Thus, it is concluded that Vitamin D is an important supplement for many aspects of PCOS including:
- Insulin resistance
- Fertility
- Hyperandrogenism
- Mood
So, one should take 5000 IU at any time of day, with or without food. Considering that proper interventions could improve outcomes of PCOS and its related complications.
We aimed to evaluate the effect of calcium and Vitamin D supplementations on menstrual regularity, follicle response, body mass index (BMI) and hyperandrogenism symptoms in women with PCOS.
Authors: Soha Navaid, Haseeb Anwar, Ghulam Hussain, Humaira Muzaffar, Arsalan Shaukat, Imtiaz Mustafa, Saima Malik, Rameen Ishfaq
Department of Physiology, Government College University, Faisalabad-Pakistan